Your Single Partner for Supplemental Benefits and Beyond
Power every benefit including flex card, OTC, meals, grocery, dental, fitness, and more through one connected platform. Lynx delivers a seamless, branded member experience with integrated rewards & incentives and care gap closure tools that can be embedded within your health plan apps or built as an extension of them.
Request a Demo
WHY LYNX
One Platform, Endless Possibilities
Lynx is a one-stop shop for supplemental benefits, and more. We provide a programmable infrastructure that brings payment flexibility, partner connectivity, and benefit control into one seamless system
- Intelligent Payments
- Centralized Benefits Hub
- Embedded Rewards
- Centralized Administration
Flexible, Programmable Payments
Lynx combines real-time spend controls with the industry’s most flexible payment capabilities, empowering health plans to tailor every transaction and benefit experience. This flexibility allows plans to design programs that are both compliant and highly personalized, giving members seamless access to all their benefit dollars in one place.
- Accepted at 70,000+ in-store locations nationwide for SKU-restricted payments, including major national and independent pharmacies and supermarkets
- Restrict Dental, Vision, and Hearing benefits down to CDT-code precision
- Support electronic payments for ancillary benefits such as utilities, transportation, and home-based services
- Run rewards & incentives on the same card and ledger as other benefits
- Manage eligibility, funding, and adjudication in real time
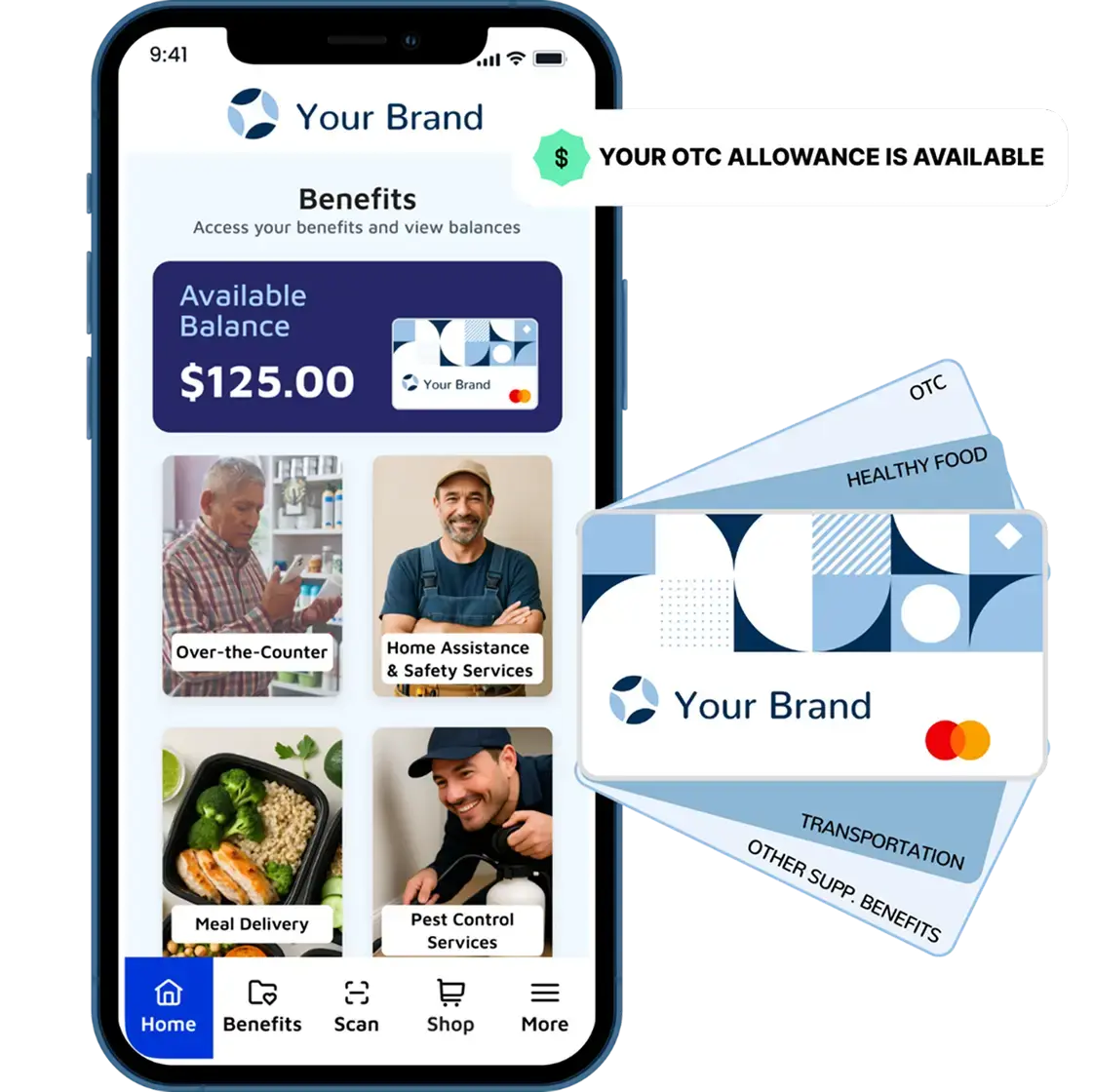
A Unified OTC and Benefits Marketplace
Lynx makes it easy for members to shop and redeem benefits through a single, branded experience. From over-the-counter (OTC) and durable medical equipment (DME) fulfillment through Fortune 10 partners to integrated networks for food, transportation, and fitness, Lynx consolidates the entire supplemental benefits ecosystem.
Lynx combines Fortune 10–backed e-commerce fulfillment with a national partner marketplace to power every aspect of supplemental benefits. Members can order OTC, DME, and grocery items, access integrated pharmacy services, and connect to trusted networks for healthy food, transportation, fitness, and dental, vision, and hearing (DVH) benefits, all managed through one centralized experience.
- Built-in fulfillment for OTC, groceries, DME, and other eligible products through Fortune 10 partners
- Pre-vetted marketplace spanning healthy food, grocery delivery, transportation, DVH, fitness, and pharmacy
- Seamless member experience with integrated checkout and single sign-on within plan-branded apps or portals
- Centralized data, reporting, and compliance oversight across all partners and fulfillment channels
- Flexible integration with your existing preferred vendors to unify operations and the member experience
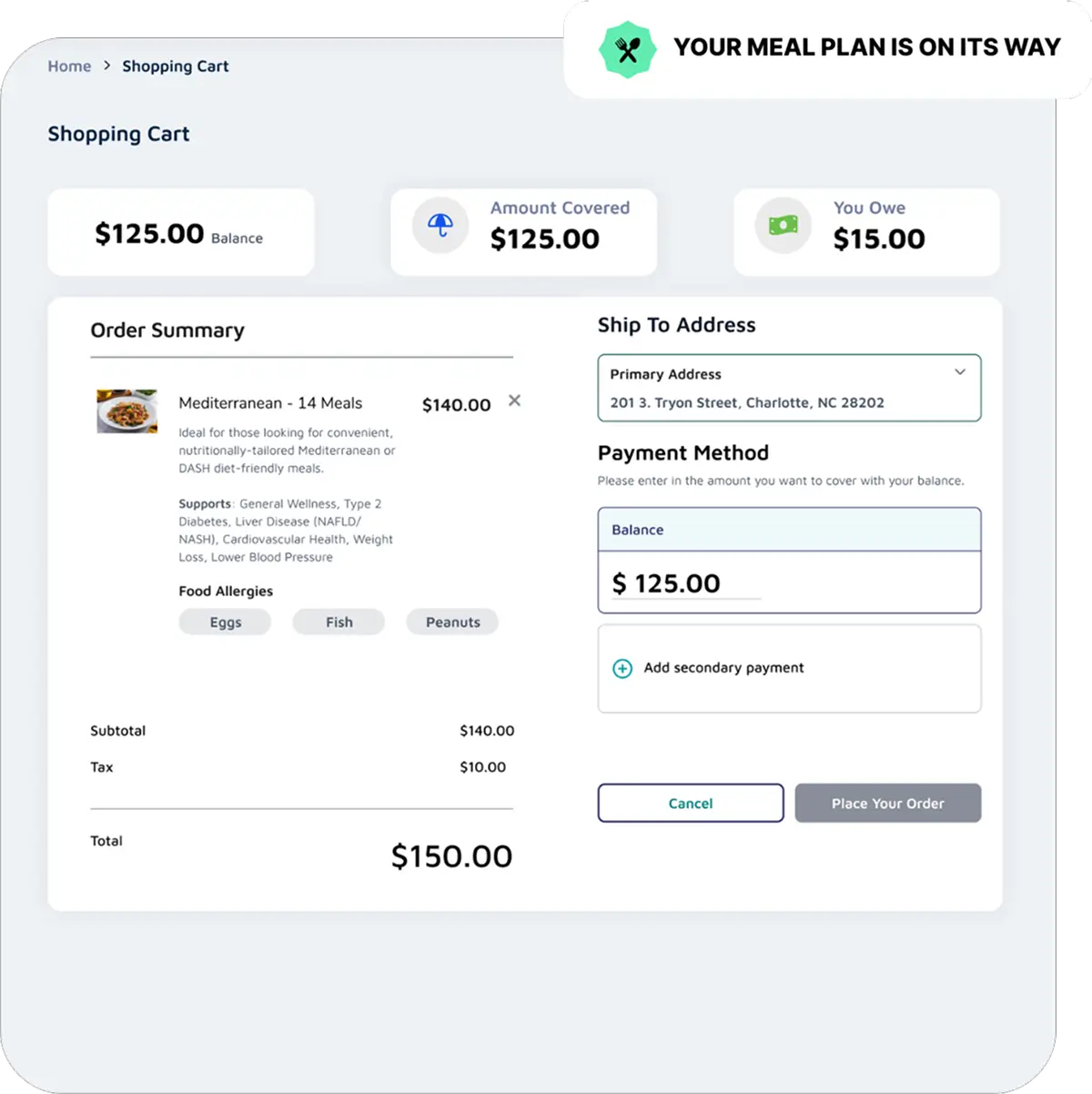
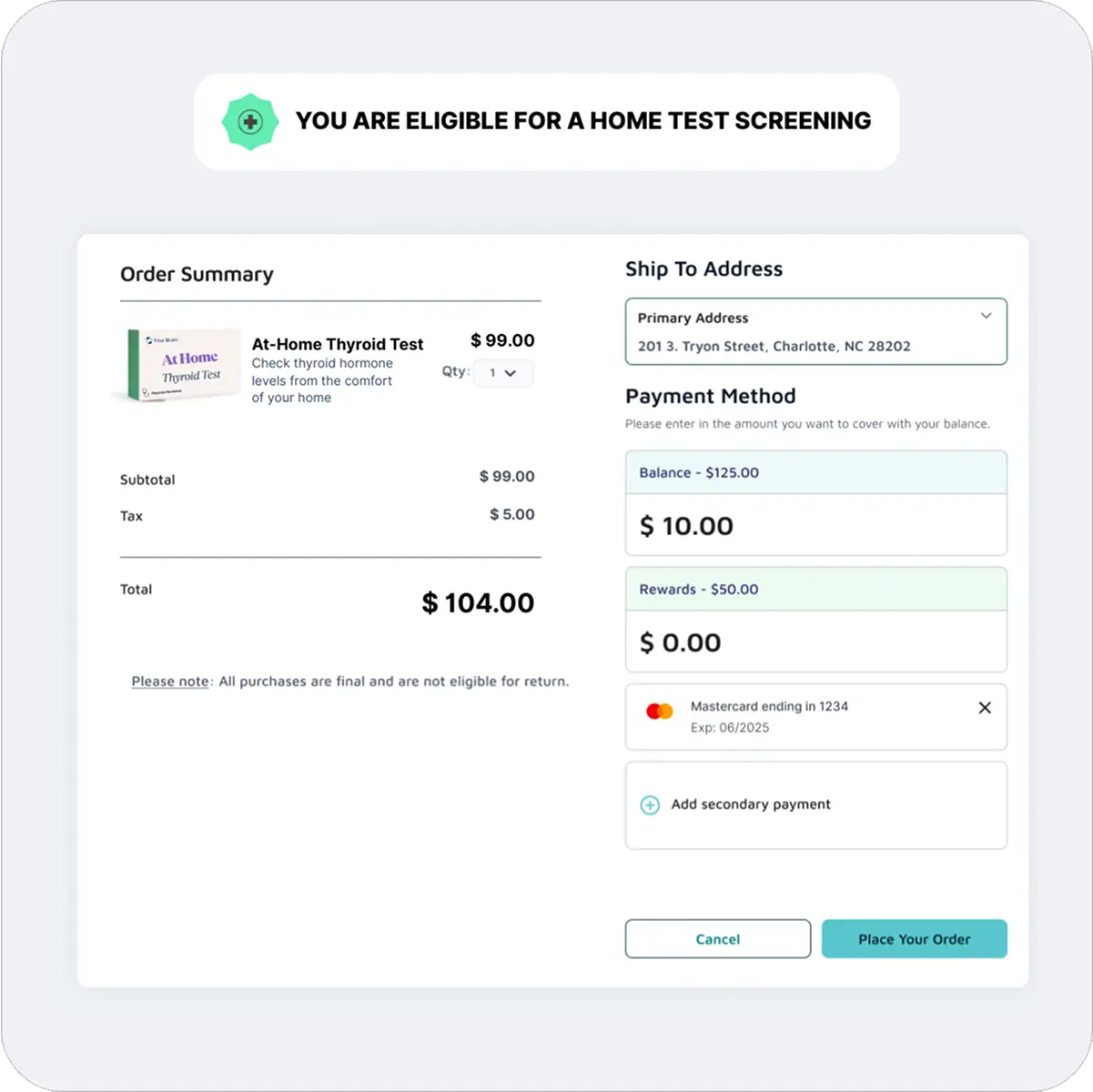
Embedded Rewards & Incentives plus Care Gap Closures
Lynx partners with Quality and Risk teams to embed rewards & incentives directly within the supplemental benefits experience, driving measurable engagement and outcomes. Members can earn and redeem rewards instantly for completing healthy actions such as screenings, preventive visits, or at-home assessments, all within the same branded environment where they manage their benefits. Lynx delivers a complete closed-loop framework for care gap closure, from enrolling members in lab tests and capturing results within the administrative platform to helping members schedule in-home or virtual assessments through a single, seamless experience.
Highlights:
- Embedded rewards & incentives within the supplemental benefits experience for higher member engagement
- One platform, one experience with no separate programs or vendors required
- Configurable incentives tied to screenings, preventive care, or chronic condition management
- Closed-loop care gap support from enrollment through result capture and follow-up
- Real-time tracking of engagement, completion, balances, and redemptions
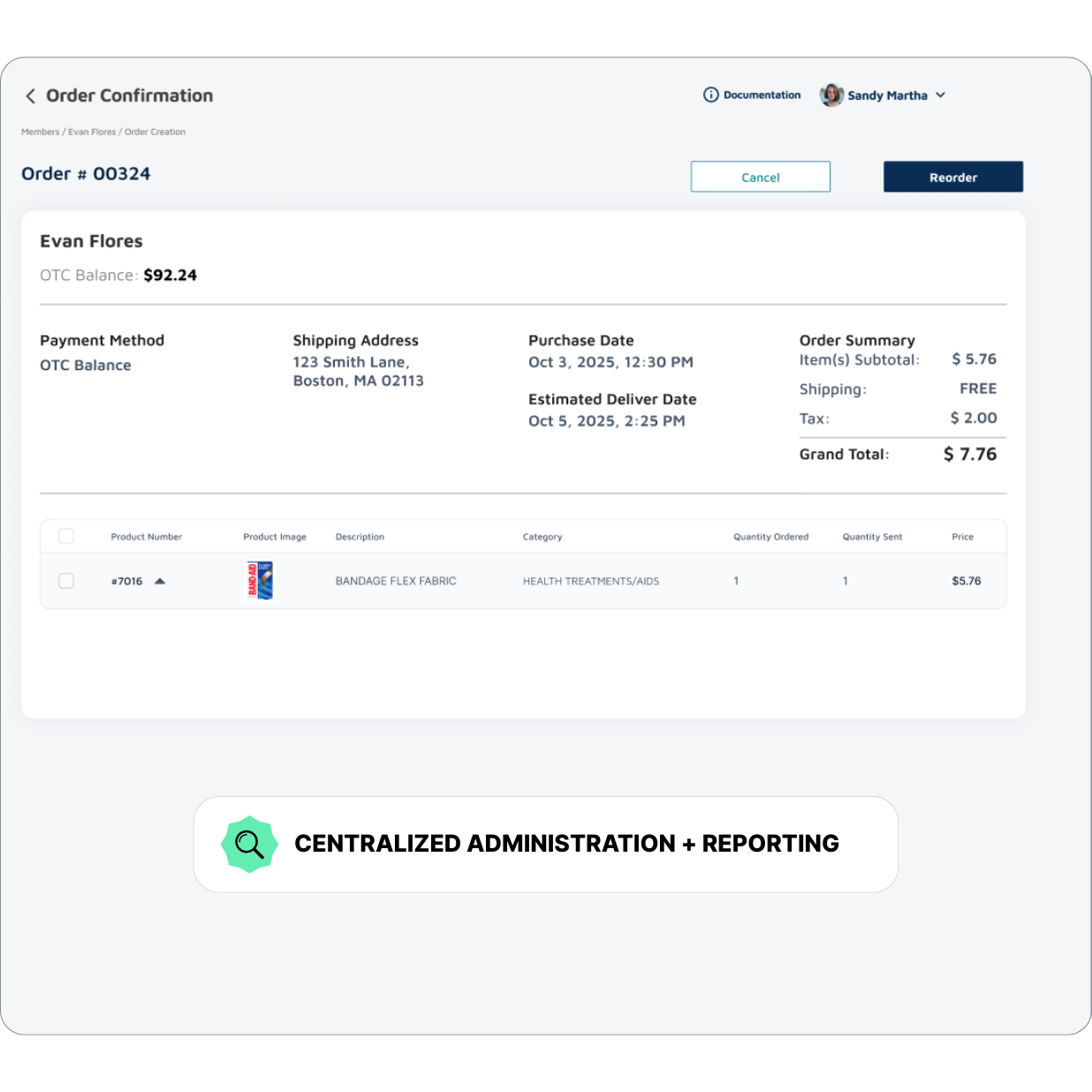
A Single Administration & Reporting Partner
Lynx eliminates the need for multiple vendor portals by centralizing administration and reporting for all supplemental benefit programs in one place. Medicare Advantage teams no longer need to navigate five to ten separate systems to understand utilization, engagement, or funding performance. Lynx delivers a single, unified view across every benefit, reward, and care gap program. Administrators can track utilization and engagement in real time, manage funding and compliance, and access consolidated analytics to drive better decisions and outcomes. The result is simplified oversight, improved transparency, and a more efficient operational model for every plan partner.
Highlights:
- One centralized platform for all benefit, rewards & incentives, and care gap reporting
- Real-time analytics to monitor utilization, participation, and performance
- Single source of truth that replaces multiple vendor portals and fragmented data
- Automated compliance oversight and audit-ready documentation
- Actionable insights connecting utilization to engagement and outcomes
Legacy systems created the problem.
Lynx solves it.
Health plans have spent years balancing compliance, innovation, and experience across a maze of outdated vendors and disconnected systems. The result is complexity, friction, and missed opportunities to engage members.
Lynx ends that cycle.
One partner. One experience. Endless flexibility to build differentiated benefit programs that work for every member, every time.
THE LYNX DIFFERENCE
From Complexity to Measurable ROI
One platform, one partner—streamlined administration and stronger member engagement
- $Millions in redundant administrative fees spread across multiple vendor contracts
- High operational costs from managing disconnected benefit, fulfillment, and reporting systems
- Limited purchasing power and higher per-member product pricing
- Fragmented member experience across digital, card, and call center channels
- Little visibility into ROI or ability to connect benefit spend to care gap closure
- $Millions in annual savings through vendor consolidation and unified administration
- Streamlined operations with one platform managing all supplemental benefits, rewards & incentives, and care gap programs
- Greater member purchasing power through direct Fortune 10 fulfillment and optimized pricing
- Integrated partner marketplace to activate new benefits, food, transportation, or fitness programs without additional vendor costs
- Closed-loop care gap tracking that connects utilization and outcomes to measurable ROI